India Medical Coding Market Size & Share - Growth Forecast Report (2026-2035)
Industry Insight by Classification System (International Classification of Diseases (ICD), Current Procedural Terminology (CPT), Healthcare Common Procedure Coding System (HCPCS), Systematized Nomenclature of Medicine – Clinical Terms (SNOMED CT)), by Offering (Outsourced Medical Coding Services, In-house Medical Coding Services, Medical Coding Software and Automation Tools), by Delivery Mode (Cloud-based Coding Solutions, On-premise Coding Systems), by Application (Radiology Coding, Oncology Coding, Cardiology Coding, Pathology Coding, Surgery / Procedure Coding), by Function (Code Assignment and Validation, Analytics and Reporting, Compliance and Audit Management, Revenue Cycle Optimization, Data Quality Management), by End User (Hospitals and Large Healthcare Facilities, Physician Practices, Clinics, and Diagnostic Centers, Insurance Providers and Payers, Specialty and Ambulatory Care Centers)
| Status : Published | Published On : Mar, 2026 | Report Code : VRHC1330 | Industry : Healthcare | Available Format :
|
Page : 141 |
India Medical Coding Market Overview
The India medical coding market which was valued at approximately USD 0.46 billion in 2025 and is estimated to rise further up to almost USD 0.52 billion by 2026, is projected to reach around USD 1.42 billion in 2035, expanding at a CAGR of about 11% during the forecast period from 2026 to 2035.
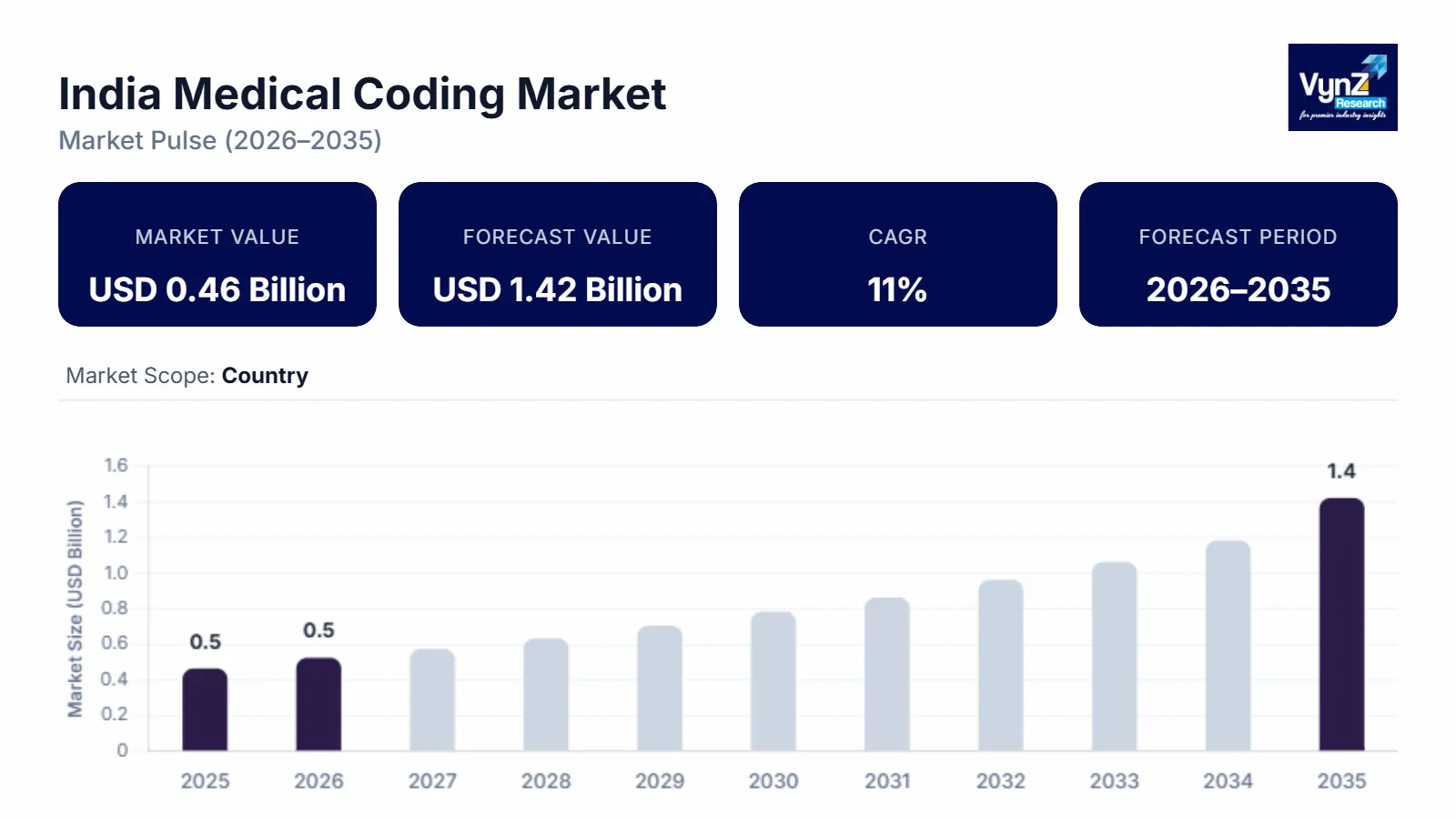
The market is growing steadily with the main drivers being increasing hospitalization rates, rising health insurance penetration, and greater outsourcing demand from international healthcare providers looking for cheaper documentation services. The advent of disease classification standardization and structured reimbursement have therefore equipped hospitals and revenue cycle management providers with the necessary tools to enhance work efficiency and hence revenue generation.
The World Health Organization highlights the necessity of standardized International Classification of Diseases systems not only for proper monitoring of the diseases but also for fair reimbursement, which is indirectly supporting the professional coding demand. The growth of multispecialty hospitals and the adoption of electronic health records in the cities of Bengaluru, Hyderabad, and Chennai are the factors that have accelerated structured documentation practices and created a less volatile market scenario.
India Medical Coding Market Dynamics
Market Trends
The industry is currently undergoing a major transformation which results in organizations adopting digital methods to create their documents and use common coding systems that follow national digital health standards. The National Digital Health Mission programs establish the essential framework which requires organizations to create electronic health records and facilitate data sharing between different systems while using standard patient identifiers to establish their documentation requirements. The World Health Organization requires healthcare institutions to establish consistent coding practices because they need to use updated International Classification of Diseases frameworks for tracking diseases and dealing with reimbursement matters. Healthcare organizations use automated coding tools together with artificial intelligence documentation review and audit analysis systems to improve their claim processing accuracy while achieving better compliance results.
Growth Drivers
The market in India benefits from the increasing number of health insurance policyholders together with the rising number of hospital admissions which occur in both public and private medical facilities. The Ayushman Bharat program has seen increased claim processing which requires extra documentation and reimbursement verification according to the National Health Authority. The Ministry of Health and Family Welfare has increased its funding for hospital infrastructure and digital health technology, which has created extra demand for coding services. International healthcare organizations are expanding their outsourcing operations because they want to find affordable experienced coding staff members, which is leading to increased revenue from international service exports. The healthcare sector will continue to need certified coding experts because organizations need to meet compliance requirements while maximizing revenue and producing standardized reports.
Market Restraints / Challenges
The market experiences operational obstacles because there is a shortage of skilled workers and complex regulatory requirements despite the strong existing demand. Standardized coding requires ongoing education which must match the International Classification of Diseases updates that the World Health Organization issues, resulting in continuous expenses for certification and skills enhancement. Advanced coding software and audit systems remain out of reach for smaller healthcare facilities because their budget restrictions prevent them from acquiring such digital transition tools. Service providers who rely on offshore contracts to serve external clients face risks from international reimbursement policy changes and currency exchange rate fluctuations. Economic downturns and regulatory changes will create difficulties for organizations to scale their operations and maintain profitability because of the existing structural limitations.
Market Opportunities
The expansion of digital coding solutions which link to electronic health record systems under national health digitalization programs creates important business opportunities. High accuracy coding and analytics services will experience continuing market demand because of the increasing interoperability requirements and the establishment of structured health data registries. The expansion of medical tourism and the growth of multispecialty tertiary hospitals in metropolitan areas like Bengaluru and Hyderabad are leading to increased documentation requirements which need standardized evaluation procedures. Healthcare providers can use artificial intelligence capacity for coding validation and automation of audit functions to boost productivity while decreasing errors, which lets them build both domestic and international compliant services and long-term partnerships with healthcare institutions.
India Medical Coding Market Report Coverage
|
Report Metric |
Details |
|
Historical Period |
2020 - 2024 |
|
Base Year Considered |
2025 |
|
Forecast Period |
2026 - 2035 |
|
Market Size in 2025 |
USD 0.46 Billion |
|
Revenue Forecast in 2035 |
USD 1.42 Billion |
|
Growth Rate |
11% |
|
Segments Covered in the Report |
Classification System, Offering, Delivery Mode, Application, Function, End User |
|
Report Scope |
Market Trends, Drivers, and Restraints; Revenue Estimation and Forecast; Segmentation Analysis; Companies’ Strategic Developments; Market Share Analysis of Key Players; Company Profiling |
|
Regions Covered in the Report |
South India, West India, North India, East India, Northeast India |
|
Key Companies |
Access Healthcare, AGS Health, CorroHealth, e-care India, Eli Global / Etransmedia, GeBBS Healthcare Solutions, Infinit Healthcare, iMarque Solutions, MedBillingExperts, Omega Healthcare |
|
Customization |
Available upon request |
India Medical Coding Market Segmentation
By Classification System
The International Classification of Diseases (ICD) segment accounted for the largest share of the India medical coding market in 2025, representing approximately 48% of total revenue. The dominance of this segment is attributed to its mandatory use for morbidity reporting, insurance claims processing, and public health surveillance under guidelines established by the World Health Organization. Hospitals, diagnostic laboratories, and insurance administrators rely on ICD codes to standardize disease classification and ensure accurate reimbursement documentation. The expansion of national digital health infrastructure and standardized reporting requirements is expected to support the continued adoption of ICD coding across healthcare systems.
The Current Procedural Terminology (CPT) segment is projected to register the fastest growth, with an estimated CAGR of 11.6% between 2026 and 2035. Growth in this segment is driven by increasing volumes of outpatient procedures, rising surgical documentation requirements, and expanding participation of Indian coding firms in global healthcare outsourcing contracts. Healthcare providers are also adopting CPT coding frameworks to align with international billing standards and improve procedural documentation.
By Offering
Outsourced medical coding services held the largest share of the India medical coding market in 2025, accounting for approximately 55% of total revenue. The segment’s dominance is supported by India’s well-established healthcare outsourcing ecosystem and the availability of a large pool of trained and certified medical coders. International hospitals, insurance companies, and revenue cycle management providers increasingly outsource coding operations to India to reduce operational costs while maintaining documentation accuracy. The growth of offshore coding contracts and integration with revenue cycle management services is expected to support this segment’s expansion at an estimated CAGR of 11.3% through 2035.
The in-house coding services segment is expected to grow at a CAGR of approximately 12.1% during the forecast period. Large hospital networks and multi-specialty healthcare institutions are strengthening internal coding teams to maintain better control over patient data and clinical documentation. Hospitals are also investing in AI-enabled coding software and automated validation tools to improve operational efficiency and reduce claim denials.
By Delivery Mode
The cloud-based medical coding solutions segment accounted for the largest share of the India medical coding market in 2025, representing approximately 54% of total deployment revenue. Healthcare providers increasingly adopt cloud-based systems because they allow scalable data storage, remote access, and seamless integration with electronic health record platforms. Government initiatives supporting digital healthcare infrastructure, including programs such as the Ayushman Bharat Digital Mission, are accelerating the adoption of interoperable cloud-based health information systems.
The on-premise deployment segment is expected to grow at a CAGR of around 11.5% between 2026 and 2035. Large hospitals and healthcare networks often prefer on-premise systems because they provide greater control over patient data security and compliance with internal IT policies. Healthcare institutions managing large volumes of insurance claims and patient documentation continue to rely on on-premise systems to ensure secure data storage and integration with existing hospital information systems.
By Application
The radiology coding segment held the largest share of the application market in 2025, accounting for approximately 37% of segment revenue. Diagnostic imaging services such as CT scans, MRI scans, and ultrasound examinations generate high volumes of coding requirements due to their frequent use in clinical diagnostics and insurance reimbursement processes. The rapid expansion of diagnostic imaging infrastructure across urban and semi-urban healthcare facilities continues to drive strong demand for radiology coding services.
The oncology coding segment is projected to experience the fastest growth during the forecast period, registering an estimated CAGR of 12.4% between 2026 and 2035. Rising cancer incidence rates, expanding oncology departments in major hospitals, and the adoption of specialized treatment protocols are contributing to increased demand for accurate coding and documentation. Government programs supporting cancer screening and treatment initiatives are also expected to increase the volume of oncology-related medical documentation.
By Function
The code assignment and validation segment accounted for the largest share of the India medical coding market in 2025, generating approximately 49% of total workflow revenue. Accurate code assignment is essential for ensuring proper insurance claims processing and compliance with clinical documentation standards. Hospitals and outsourcing providers rely on certified coders and automated validation systems to minimize claim errors and improve reimbursement outcomes.
The analytics and reporting segment is expected to register the fastest growth, with an estimated CAGR of 12.2% during the forecast period. Healthcare providers are increasingly adopting data analytics tools to monitor coding performance, track reimbursement trends, and optimize revenue cycle management processes. The growing emphasis on healthcare data management and regulatory reporting requirements is encouraging healthcare institutions to integrate advanced analytics platforms into their coding workflows.
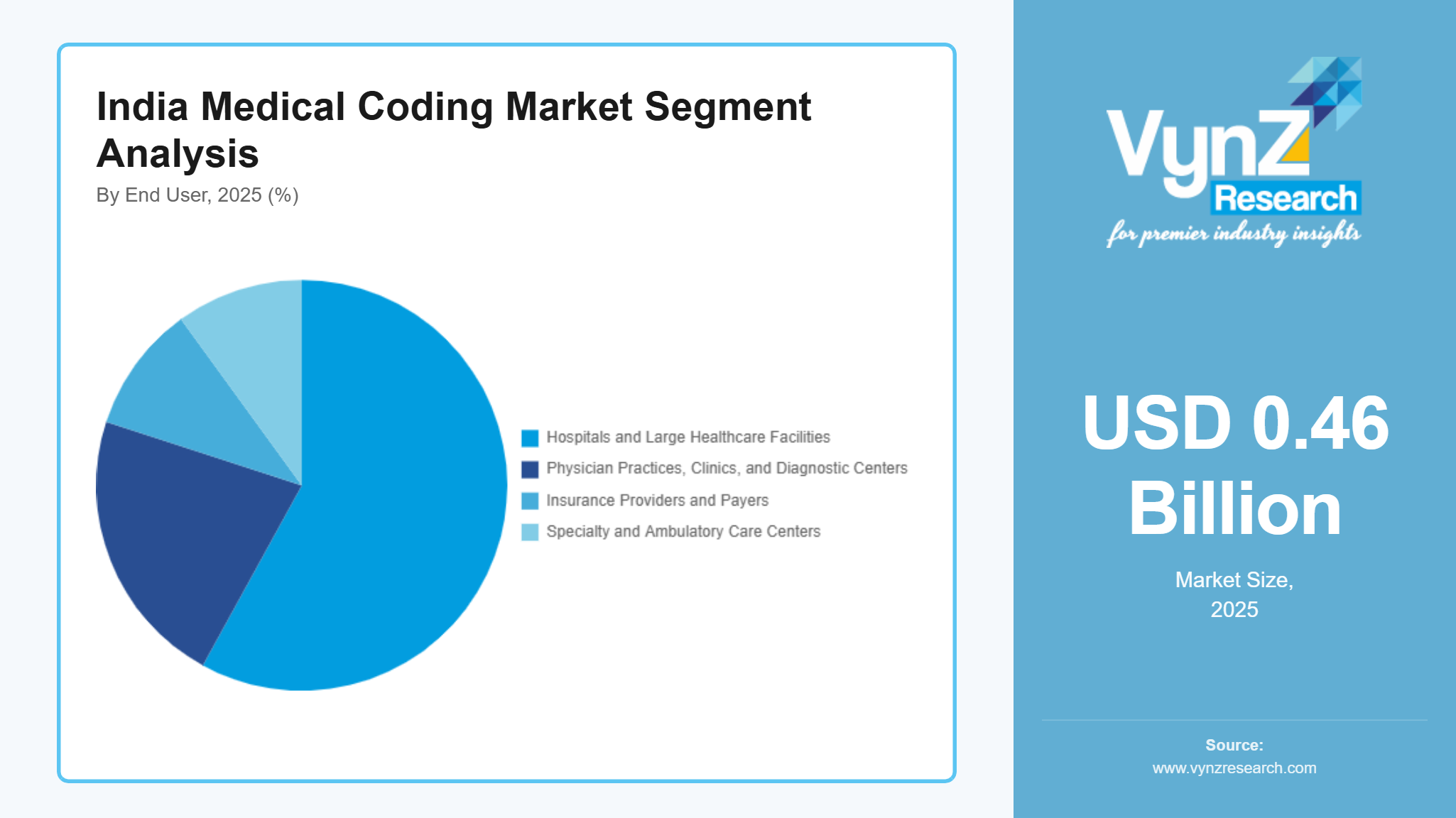
By End User
The hospitals and large healthcare facilities segment dominated the India medical coding market in 2025, accounting for approximately 58% of total demand. Hospitals handle a high volume of inpatient and outpatient procedures, which require complex coding for insurance claims and reimbursement processing. The expansion of hospital infrastructure supported by the Ministry of Health and Family Welfare (India) and the increasing number of claims processed under public insurance programs are key factors driving demand for coding services in this segment.
The physician practices, clinics, and diagnostic centers segment is projected to grow at the fastest pace, with an estimated CAGR of 11.8% between 2026 and 2035. The increasing adoption of digital health records, expansion of outpatient care services, and growing diagnostic testing demand are encouraging smaller healthcare facilities to adopt medical coding solutions. Many clinics and diagnostic centers are also utilizing outsourced coding services and cloud-based platforms to improve billing accuracy and operational efficiency.
Regional Insights
South India
The market received 32% of its market share from South India in 2025. The region achieved this success because it had both healthcare IT service providers and established private hospital facilities and international healthcare outsourcing partnerships. The cities of Bengaluru, Hyderabad and Chennai operate as primary business centers because they have both qualified clinical documentation staff members and the newest digital health technologies. The Ministry of Health and Family Welfare leads digital health projects which the government supports. These projects achieve their goals through ISO-standard disease classification systems which fundamental World Health Organization methods mandate hospitals to use for structured coding development. The region experiences increasing demand because more people acquire insurance and file a higher number of claims.
West India
The West Indian market reached 24% of its total size in 2025 because the expansion of hospital networks, medical tourism and health insurance penetration has created new business opportunities. The two cities of Mumbai and Pune function as major healthcare centers because hospitals there have established private healthcare systems which need revenue cycle management services. National health assurance programs have implemented policies that help hospitals digitize their systems. These programs establish common standards which lead to better documentation performance through improved compliance. The healthcare sector maintains its regional growth through electronic health records and coding automation tools. Tertiary hospitals and diagnostic chains use these systems to create organized coding services which help their business operations.
North India
North India contributes 21% of market revenue because public healthcare funding has increased. The region has expanded hospital capacity and more people now receive government health insurance benefits. The growing service centers in Delhi NCR and Noida and Gurugram connect nearby hospital networks with large hospital groups and administrative institutions. The national health authorities have established reimbursement guidelines which require hospitals to use specific documentation procedures. The eastern and northeastern regions of the market hold 23% even with limited adoption because their infrastructure and workforce development process has not yet reached sufficient levels.
Competitive Landscape / Company Insights
The market operates with moderate competition because domestic service providers and global revenue cycle management companies compete through their workforce development, process automation and compliance service delivery methods. Companies are developing AI-based coding platforms, audit analytics and training programs which follow World Health Organization standardized disease classification systems. Providers will improve their operational accuracy and system scalability through government-supported digital health programs and insurance claim standardization initiatives which will also help them build stronger partnerships with institutions for extended periods.
Mini Profiles
Access Healthcare focuses on revenue cycle management, medical coding, and analytics, supported by global delivery centers and strong payer-provider relationships that enhance operational efficiency and scalable cost advantages worldwide sustainable.
CorroHealth operates in niche healthcare compliance and audit segments, emphasizing technology-enabled risk adjustment, coding accuracy, and value-based care solutions to improve reimbursement integrity and documentation performance for providers and plans.
e-care India leverages digital reach and offshore delivery infrastructure to expand market presence, providing medical billing, coding, and practice management services with competitive pricing and customized support for healthcare clients.
GeBBS Healthcare Solutions operates in mass and mid-market segments, emphasizing process optimization, automation, and analytics-driven revenue cycle services supported by strong client retention, scalable platforms, and diversified global delivery capabilities.
Omega Healthcare focuses on end-to-end revenue cycle management, supported by extensive global workforce, strategic partnerships, and cost-efficient offshore centers that strengthen brand recognition and long-term provider relationships across healthcare markets.
Key Players
- Access Healthcare
- AGS Health
- CorroHealth
- e-care India
- Eli Global / Etransmedia
- GeBBS Healthcare Solutions
- Infinit Healthcare
- iMarque Solutions
- MedBillingExperts
- Omega Healthcare
Recent Developments
In March 2026, a formal commercial agreement between SuperDial, a healthcare automation platform that streamlines payer and provider outreach operations, and Omega Healthcare, an AI-driven healthcare solutions firm, was announced today. By integrating with SuperDial's voice AI automation service, Omega Healthcare will improve its agentic AI platform and assist clients in lowering administrative costs and speeding up time to cash. Under the partnership, SuperDial will work closely with Omega Healthcare to be incorporated into the company’s agentic AI platform, which puts intelligence into action by providing voice automation to deliver measurable revenue cycle operations outcomes for Omega Healthcare’s customers.
In July 2025, the public and private sectors of Malaysia, Infinity Medical is establishing itself as a major supplier of affordable neonatal critical care solutions which was announced during the event, The Health Industry Series – ASEAN 2025 in Malaysia. The company offer cutting-edge yet reasonably priced equipment.
In June 2025, US-based CorroHealth has made a "strategic" investment in UAE-based healthtech company SANTECHTURE. The investment formalizes a two-year partnership between the two businesses, which have co-hosted industry events including the Arab Health 2025 reception and implemented AI-driven RCM technologies for local clients.
India Medical Coding Market Coverage
Classification System Insight and Forecast 2026 - 2035
- International Classification of Diseases (ICD)
- Current Procedural Terminology (CPT)
- Healthcare Common Procedure Coding System (HCPCS)
- Systematized Nomenclature of Medicine – Clinical Terms (SNOMED CT)
Offering Insight and Forecast 2026 - 2035
- Outsourced Medical Coding Services
- In-house Medical Coding Services
- Medical Coding Software and Automation Tools
Delivery Mode Insight and Forecast 2026 - 2035
- Cloud-based Coding Solutions
- On-premise Coding Systems
Application Insight and Forecast 2026 - 2035
- Radiology Coding
- Oncology Coding
- Cardiology Coding
- Pathology Coding
- Surgery / Procedure Coding
Function Insight and Forecast 2026 - 2035
- Code Assignment and Validation
- Analytics and Reporting
- Compliance and Audit Management
- Revenue Cycle Optimization
- Data Quality Management
End User Insight and Forecast 2026 - 2035
- Hospitals and Large Healthcare Facilities
- Physician Practices
- Clinics
- and Diagnostic Centers
- Insurance Providers and Payers
- Specialty and Ambulatory Care Centers
India Medical Coding Market by Region
- South India
- By Classification System
- By Offering
- By Delivery Mode
- By Application
- By Function
- By End User
- West India
- By Classification System
- By Offering
- By Delivery Mode
- By Application
- By Function
- By End User
- North India
- By Classification System
- By Offering
- By Delivery Mode
- By Application
- By Function
- By End User
- East India
- By Classification System
- By Offering
- By Delivery Mode
- By Application
- By Function
- By End User
- Northeast India
- By Classification System
- By Offering
- By Delivery Mode
- By Application
- By Function
- By End User
Table of Contents for India Medical Coding Market Report
1. Research Overview
1.1. The Report Offers
1.2. Market Coverage
1.2.1. By
Classification System
1.2.2. By
Offering
1.2.3. By
Delivery Mode
1.2.4. By
Application
1.2.5. By
Function
1.2.6. By
End User
1.3. Research Phases
1.4. Limitations
1.5. Market Methodology
1.5.1. Data Sources
1.5.1.1.
Primary Research
1.5.1.2.
Secondary Research
1.5.2. Methodology
1.5.2.1.
Data Exploration
1.5.2.2.
Forecast Parameters
1.5.2.3.
Data Validation
1.5.2.4.
Assumptions
1.5.3. Study Period & Data Reporting Unit
2. Executive Summary
3. Industry Overview
3.1. Industry Dynamics
3.1.1. Market Growth Drivers
3.1.2. Market Restraints
3.1.3. Key Market Trends
3.1.4. Major Opportunities
3.2. Industry Ecosystem
3.2.1. Porter’s Five Forces Analysis
3.2.2. Recent Development Analysis
3.2.3. Value Chain Analysis
3.3. Competitive Insight
3.3.1. Competitive Position of Industry
Players
3.3.2. Market Attractive Analysis
3.3.3. Market Share Analysis
4. India Market Estimate and Forecast
4.1. India Market Overview
4.2. India Market Estimate and Forecast to 2035
5. Market Segmentation Estimate and Forecast
5.1. By Classification System
5.1.1. International Classification of Diseases (ICD)
5.1.1.1. Market Definition
5.1.1.2. Market Estimation and Forecast to 2035
5.1.2. Current Procedural Terminology (CPT)
5.1.2.1. Market Definition
5.1.2.2. Market Estimation and Forecast to 2035
5.1.3. Healthcare Common Procedure Coding System (HCPCS)
5.1.3.1. Market Definition
5.1.3.2. Market Estimation and Forecast to 2035
5.1.4. Systematized Nomenclature of Medicine – Clinical Terms (SNOMED CT)
5.1.4.1. Market Definition
5.1.4.2. Market Estimation and Forecast to 2035
5.2. By Offering
5.2.1. Outsourced Medical Coding Services
5.2.1.1. Market Definition
5.2.1.2. Market Estimation and Forecast to 2035
5.2.2. In-house Medical Coding Services
5.2.2.1. Market Definition
5.2.2.2. Market Estimation and Forecast to 2035
5.2.3. Medical Coding Software and Automation Tools
5.2.3.1. Market Definition
5.2.3.2. Market Estimation and Forecast to 2035
5.3. By Delivery Mode
5.3.1. Cloud-based Coding Solutions
5.3.1.1. Market Definition
5.3.1.2. Market Estimation and Forecast to 2035
5.3.2. On-premise Coding Systems
5.3.2.1. Market Definition
5.3.2.2. Market Estimation and Forecast to 2035
5.4. By Application
5.4.1. Radiology Coding
5.4.1.1. Market Definition
5.4.1.2. Market Estimation and Forecast to 2035
5.4.2. Oncology Coding
5.4.2.1. Market Definition
5.4.2.2. Market Estimation and Forecast to 2035
5.4.3. Cardiology Coding
5.4.3.1. Market Definition
5.4.3.2. Market Estimation and Forecast to 2035
5.4.4. Pathology Coding
5.4.4.1. Market Definition
5.4.4.2. Market Estimation and Forecast to 2035
5.4.5. Surgery / Procedure Coding
5.4.5.1. Market Definition
5.4.5.2. Market Estimation and Forecast to 2035
5.5. By Function
5.5.1. Code Assignment and Validation
5.5.1.1. Market Definition
5.5.1.2. Market Estimation and Forecast to 2035
5.5.2. Analytics and Reporting
5.5.2.1. Market Definition
5.5.2.2. Market Estimation and Forecast to 2035
5.5.3. Compliance and Audit Management
5.5.3.1. Market Definition
5.5.3.2. Market Estimation and Forecast to 2035
5.5.4. Revenue Cycle Optimization
5.5.4.1. Market Definition
5.5.4.2. Market Estimation and Forecast to 2035
5.5.5. Data Quality Management
5.5.5.1. Market Definition
5.5.5.2. Market Estimation and Forecast to 2035
5.6. By End User
5.6.1. Hospitals and Large Healthcare Facilities
5.6.1.1. Market Definition
5.6.1.2. Market Estimation and Forecast to 2035
5.6.2. Physician Practices
5.6.2.1. Market Definition
5.6.2.2. Market Estimation and Forecast to 2035
5.6.3. Clinics
5.6.3.1. Market Definition
5.6.3.2. Market Estimation and Forecast to 2035
5.6.4. and Diagnostic Centers
5.6.4.1. Market Definition
5.6.4.2. Market Estimation and Forecast to 2035
5.6.5. Insurance Providers and Payers
5.6.5.1. Market Definition
5.6.5.2. Market Estimation and Forecast to 2035
5.6.6. Specialty and Ambulatory Care Centers
5.6.6.1. Market Definition
5.6.6.2. Market Estimation and Forecast to 2035
6. South India Market Estimate and Forecast
6.1. By
Classification System
6.2. By
Offering
6.3. By
Delivery Mode
6.4. By
Application
6.5. By
Function
6.6. By
End User
7. West India Market Estimate and Forecast
7.1. By
Classification System
7.2. By
Offering
7.3. By
Delivery Mode
7.4. By
Application
7.5. By
Function
7.6. By
End User
8. North India Market Estimate and Forecast
8.1. By
Classification System
8.2. By
Offering
8.3. By
Delivery Mode
8.4. By
Application
8.5. By
Function
8.6. By
End User
9. East India Market Estimate and Forecast
9.1. By
Classification System
9.2. By
Offering
9.3. By
Delivery Mode
9.4. By
Application
9.5. By
Function
9.6. By
End User
10. Northeast India Market Estimate and Forecast
10.1. By
Classification System
10.2. By
Offering
10.3. By
Delivery Mode
10.4. By
Application
10.5. By
Function
10.6. By
End User
11. Company Profiles
11.1.
Access Healthcare
11.1.1.
Snapshot
11.1.2.
Overview
11.1.3.
Offerings
11.1.4.
Financial
Insight
11.1.5.
Recent
Developments
11.2.
AGS Health
11.2.1.
Snapshot
11.2.2.
Overview
11.2.3.
Offerings
11.2.4.
Financial
Insight
11.2.5.
Recent
Developments
11.3.
CorroHealth
11.3.1.
Snapshot
11.3.2.
Overview
11.3.3.
Offerings
11.3.4.
Financial
Insight
11.3.5.
Recent
Developments
11.4.
e-care India
11.4.1.
Snapshot
11.4.2.
Overview
11.4.3.
Offerings
11.4.4.
Financial
Insight
11.4.5.
Recent
Developments
11.5.
Eli Global / Etransmedia
11.5.1.
Snapshot
11.5.2.
Overview
11.5.3.
Offerings
11.5.4.
Financial
Insight
11.5.5.
Recent
Developments
11.6.
GeBBS Healthcare Solutions
11.6.1.
Snapshot
11.6.2.
Overview
11.6.3.
Offerings
11.6.4.
Financial
Insight
11.6.5.
Recent
Developments
11.7.
Infinit Healthcare
11.7.1.
Snapshot
11.7.2.
Overview
11.7.3.
Offerings
11.7.4.
Financial
Insight
11.7.5.
Recent
Developments
11.8.
iMarque Solutions
11.8.1.
Snapshot
11.8.2.
Overview
11.8.3.
Offerings
11.8.4.
Financial
Insight
11.8.5.
Recent
Developments
11.9.
MedBillingExperts
11.9.1.
Snapshot
11.9.2.
Overview
11.9.3.
Offerings
11.9.4.
Financial
Insight
11.9.5.
Recent
Developments
11.10.
Omega Healthcare
11.10.1.
Snapshot
11.10.2.
Overview
11.10.3.
Offerings
11.10.4.
Financial
Insight
11.10.5.
Recent
Developments
12. Appendix
12.1. Exchange Rates
12.2. Abbreviations
Note: Financial insight and recent developments of different companies are subject to the availability of information in the secondary domain.
Purchase Options
Latest Report
Research Methodology
- Desk Research / Pilot Interviews
- Build Market Size Model
- Research and Analysis
- Final Deliverable
Connect With Our Sales Team
- Toll-Free: +1-888-253-3960
- Phone: +91 9960 288 381
- Email: enquiry@vynzresearch.com
India Medical Coding Market
